
Treatment Trends in Hemophilia A Interpreted from Real-World Data: Focus on Major Biologic Therapies
April 17 each year is designated as World Hemophilia Day by the World Federation of Hemophilia. This day serves as an important opportunity to raise global awareness of hemophilia and other congenital bleeding disorders, as well as to advocate for improved access to treatment.
Hemophilia A is a hereditary bleeding disorder caused by a deficiency or reduced activity of coagulation factor VIII. Repeated intra-articular bleeding can lead to hemophilic arthropathy over the long term, significantly impairing patients’ quality of life (QOL). Currently, regular prophylactic replacement therapy aimed at preventing bleeding is widely established as the standard of care. In recent years, in addition to conventional coagulation factor products, the introduction of non-factor therapies such as antibody-based agents (e.g., emicizumab) and extended half-life (EHL) products has contributed to reduced treatment burden and improved hemostatic control.
In this report, using MDV data, we analyzed trends from 2015 to 2025 in the number of patients with Hemophilia A and those receiving treatment, utilization patterns of major biologic products, and the incidence of thrombotic and embolic events following diagnosis.
1. Hemophilia A: Trends in the Number of Patients and Treated Patients
We analyzed trends in the number of patients diagnosed with Hemophilia A and those who actually received treatment.
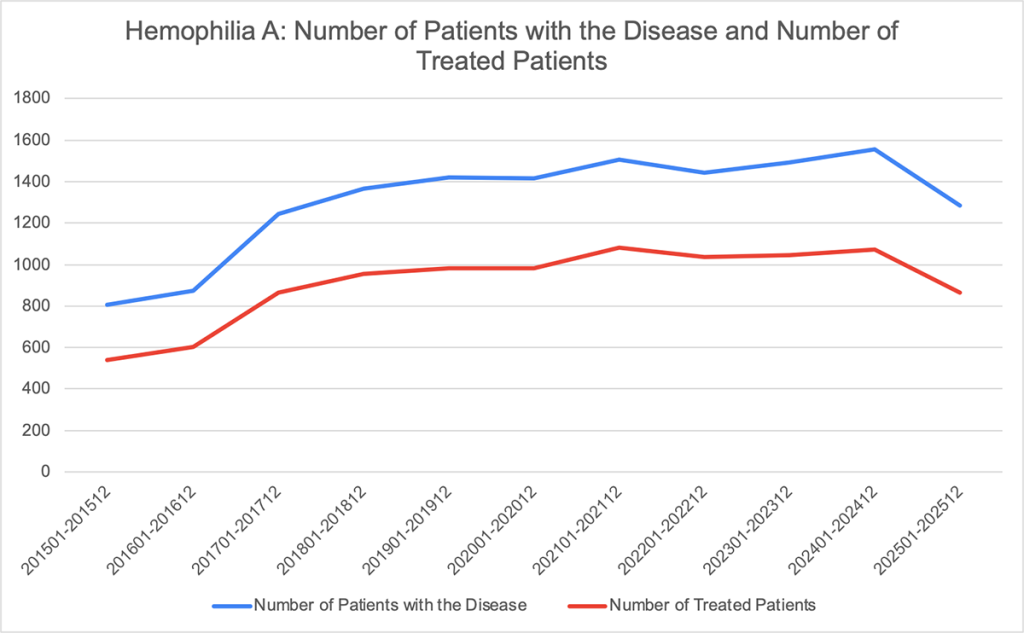
Study period: January 2015 – December 2025
Target disease: Hemophilia A
Throughout the study period, the number of diagnosed patients (blue) and treated patients (red) showed broadly parallel trends. Both indicators declined in 2025; this is likely attributable to factors such as changes in the number of facilities included in the data source.
Stable treatment rate:
A consistent gap exists between the number of diagnosed patients and those receiving treatment; however, this ratio (treatment intervention rate) remained stable over the entire period.
Background of untreated patients:
This group may include patients with mild disease not requiring regular prophylaxis, those under observation, and patients receiving on-demand treatment only at the time of bleeding events.
2. Trends in the Number of Patients Using Major Biologic Products
We analyzed trends in the number of patients using major biologic therapies for Hemophilia A, including both coagulation factor products and non-factor therapies.
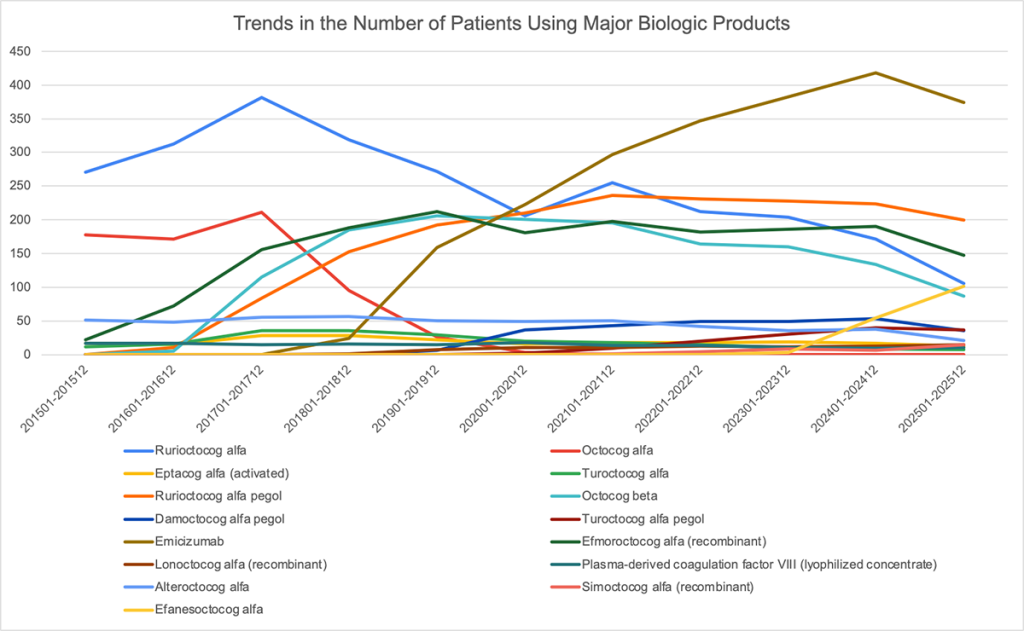
Study period: January 2015 – December 2025
Target disease: Hemophilia A
Expansion of non-factor therapy (emicizumab):
Emicizumab (brown), introduced after 2018, showed rapid growth in patient numbers and surpassed existing major therapies by 2020. By the end of 2024, it reached approximately 420 patients, the highest among all products. Although a slight decline is observed in the most recent data, it continues to represent the largest patient population.
Decline in conventional products:
Some conventional factor VIII products (e.g., rurioctocog alfa [light blue], octocog alfa [red]) peaked around 2017–2018 and subsequently declined. The reduction in patient numbers coincides with the uptake of emicizumab, suggesting a shift in treatment selection.
Trends in EHL products:
EHL products such as rurioctocog alfa pegol (orange) increased after 2016 and have since maintained a certain level of use despite fluctuations. This suggests continued utilization within specific patient populations.
Interpretation:
The concurrent increase in emicizumab use and decrease in some conventional products suggests a shift toward non-factor therapies. This represents an important trend reflecting changes in treatment selection for Hemophilia A.
3. Incidence of Thrombotic and Embolic Events After Hemophilia A Diagnosis
Given that thrombosis is an important adverse event in Hemophilia A treatment, we analyzed the incidence of thrombotic and embolic conditions following diagnosis among patients diagnosed with Hemophilia A during the period from January 2015 to December 2025.
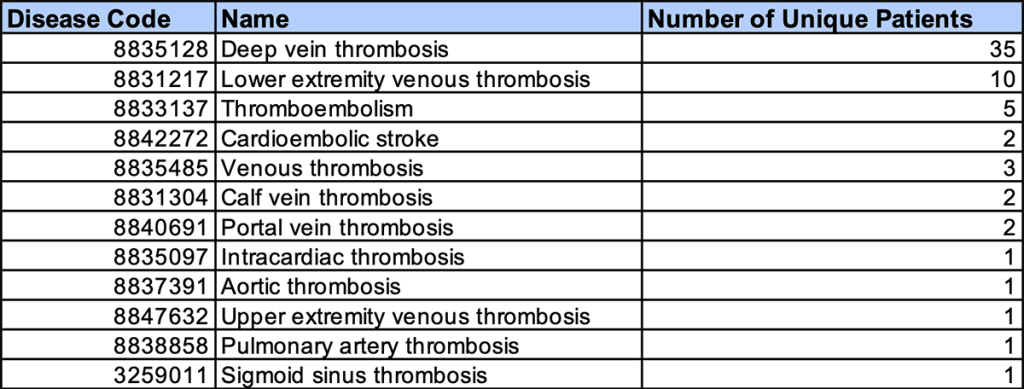
Study period: January 2015 – December 2025
Target population: Patients diagnosed with Hemophilia A (confirmed cases)
Number of patients: 1,509
Incidence trends:
Deep vein thrombosis (35 patients) was the most frequently observed condition, followed by lower extremity venous thrombosis (10 patients). A tendency toward thrombosis in the venous system, particularly in the lower extremities, was observed.
Interpretation:
It is noteworthy that a certain number of thrombotic events were identified even among patients with Hemophilia A, a bleeding disorder. These findings may be influenced by factors such as aging, an increase in comorbidities, and medical interventions including hospitalization and surgery. However, causal relationships cannot be determined based on this dataset alone. The relatively high proportion of deep vein thrombosis suggests the importance of considering thrombotic risk in addition to hemostatic management in clinical practice.
Summary
The number of patients with Hemophilia A has shown a gradual increasing trend, likely reflecting improvements in diagnosis and extended life expectancy. While coagulation factor replacement therapy remains the foundation of treatment, recent years have seen diversification in treatment options, particularly with the widespread adoption of non-factor therapies such as emicizumab, especially among patients with inhibitors. In addition, switching to EHL products has progressed, which is considered to have significant clinical value in reducing treatment burden.
Note: This article was published on April 2, 2026.
Data survey and analysis tailored to your specific requests
Databases, data analysis requests, and more.
© Medical Data Vision Co., Ltd. All Rights Reserved.





